Lower Limb Tendinopathy Symposium
Take home messages!
The Lower Limb Tendinopathy Symposium, held over September 9th and 10th weekend, hosted by Physiosports Brighton was presented by leading experts in the field of tendons, Jill Cook, Ebonie Rio and Sean Docking from La Trobe Sport and Exercise Medicine Research Centre and the long term head of the Physical Therapies Department at the Australian Institute of Sport, Professor Craig Purdam.
The first day focused on updating attendees with the latest research and clinical findings such as new research in tendinopathy, the role of pains sciences in treating tendinopathy, (1, 2) findings from imaging studies (3, 4) and revisiting the tendon continuum model.(5) The second day combined small group workshops and several case study presentations. After such great presentations, this blog aims to give the reader an enormous amount of tips and tricks in the field of lower limb tendinopathy and aims to share a few clinical pearls gained from the course.
Ultrasound Tissue Characterization (UTC) visualizes and quantifies 3-D Tendon Integrity and can discriminate various pathological stages and is highly reproducible and is a relatively new technique. Dr Sean Docking, who researches this area had several key messages;
- With increases in tendon load comes tissue
 daptation and changes to tendon structure. Currently there is limited understanding of the features of these changes which correlate to pain and disability.(4) Interestingly from his research a high proportion of asymptomatic athletes had pathology on UTC. His research shows that “directing treatment based on pathology, you are going to get it wrong 55% of the time!”
daptation and changes to tendon structure. Currently there is limited understanding of the features of these changes which correlate to pain and disability.(4) Interestingly from his research a high proportion of asymptomatic athletes had pathology on UTC. His research shows that “directing treatment based on pathology, you are going to get it wrong 55% of the time!” - Related to the previous point, clinical examination is key. For example, if you aren’t thinking the clinical symptoms are related to the tendon before imaging, don’t suddenly think that it’s tendon generated pain after observing tendon pathology on your scan!
- The extent of pathology does not direct treatment unless there is a complete tear. Think “It’s all about the doughnut not the hole!”. Pathological tendon compensates by increasing in size and in turn has “enough, if not more, ‘good’ load-bearing structure.” (3) Treatment should be focused on loading the doughnut
Craig Purdam has many years’ experience in the treatment of hamstring tendinopathy in athletes. From his experience hamstring origin tendinopathy can co-exist with sciatic nerve changes. It is therefore imperative to include both muscle and nerve/neural tests in objective examination.
- A hamstring tendinopathy will have associated hamstring and gluteal wasting on symptomatic side whereas a sciatic nerve irritation without hamstring involvement will not. Observation of muscle bulk is key both in lying and standing
- Some hamstring clinical tests that are useful include single leg bridge, both straight and bent leg and neural tests with the addition of leg adduction and internal rotation can give you a greater appreciation of nerve involvement
- Self-massage with spiky ball, in the presence of a neural component, may feel good but does not seem to help overall
Dr Ebonie Rio has focused her research on the relationship between pain science and tendinopathy. Ebonie has successfully integrated years of clinical experience at the Victorian Institute of sport, Australian Ballet Company and school and Olympic games with teaching and research. Ebonie’s work shop focused on management of Achilles tendinopathy. Key messages included;
- Make sure to clear differential diagnoses masking as Achilles tendinopathy e.g. posterior impingement, sural nerve irritation, Flexor Hallucis Longus (FHL) tenosynovitis and Tibialis posterior tendinopathy

- Checking for paratendinitis has been associated with audible crepitus of the tendon when moved through range. However a clinician may miss it. Using a stethoscope over the tendon will ensure any audible noise is not missed. (Thanks Dr. Andrew Garnham!) Think not only Achilles for this trick but also FHL, tibialis anterior and for rowers intersection syndrome in the upper limb.
- Drawing a line from the ankle to 2nd toe can provide a valuable visual feedback for patients to ensure calf raise are performed in pure sagittal plane. (Huge credit to Dr. Sue Mays (Australian Ballet Company) for her generous knowledge and expertise in not only calf rehabilitation but assessment, tips and tricks)
- When using the metronome for calf raise exercise think of x2 up and x3 beeps down. Mentrome should be set at 60 Bpm and to be effective should include auditory cues. Watch this space for a new app developed by this great team of clinical researchers.
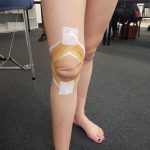
Professor Jill Cook went through a useful clinical taping technique that aims to offload the patellofemoral joint (PFJ) and may assist to differentiate pain coming from the PFJ. A diamond shape around the patella is tensioned that is proposed to slightly lift the patella away from the femoral trochlea.

The Spanish squat exercise, often used in the treatment of patellar tendinopathy, is a great way to load quadricep muscles isometrically. “Don’t use a seat belt, it will be a disaster and it will break.” This particular belt that Professor Cook uses is rated to 1000 kgs. Instructions to patient should include ‘keep body upright, arms by the side and slowly sit down.’ The knee angle should be determined by the individual and be at a point that they feel like they can hold the position for a clinician’s pre-determined time e.g. 45 seconds. Feet should be secure to avoid slipping with the attachment point needing to be onto a sturdy structure designed to handle weight.
Written by Zuzana Machotka
References
- Rio E, Kidgell D, Moseley GL, Gaida J, Docking S, Purdam C, et al. Tendon neuroplastic training: changing the way we think about tendon rehabilitation: a narrative review. Br J Sports Med. 2015:bjsports-2015-095215.
- Rio E, Moseley L, Purdam C, Samiric T, Kidgell D, Pearce AJ, et al. The pain of tendinopathy: physiological or pathophysiological? Sports medicine. 2014;44(1):9-23.
- Docking S, Cook J. Pathological tendons maintain sufficient aligned fibrillar structure on ultrasound tissue characterization (UTC). Scandinavian journal of medicine & science in sports. 2016;26(6):675-83.
- Docking SI, Ooi CC, Connell D. Tendinopathy: is imaging telling us the entire story? journal of orthopaedic & sports physical therapy. 2015;45(11):842-52.
- Cook J, Rio E, Purdam C, Docking S. Revisiting the continuum model of tendon pathology: what is its merit in clinical practice and research? Br J Sports Med. 2016:bjsports-2015-095422.