By Adam Culvenor, PT, PhD
Many people with knee pain have an MRI scan to help confirm the exact cause of pain. But how do we really know that the ‘tear’ or ‘damage’ found on an MRI is the cause of all that pain? Truth is, often it’s difficult to know. This is partly because many healthy people without any knee pain or injury will have ‘something wrong’ on their MRI – maybe this ‘something’ isn’t wrong as such, but rather a normal part of life. Just like wrinkles appear as we age, our knees undergo normal changes as we age.
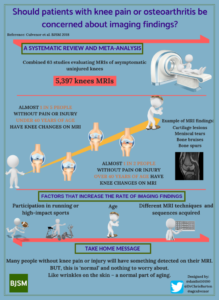
But how common are these ‘normal’ changes? This was the exact question our recent research set out to answer.
Our systematic review recently published in British Journal of Sports Medicine collated all 63 studies that evaluated the prevalence of knee osteoarthritis features on MRI in non-painful, uninjured knees (in total 5,397 knees).
Follow discussion of the paper
The prevalence of each of the MRI findings is shown in the table below, split into younger adults (<40 years old) and older adults (≥40 years old).
| Meniscus tear | Cartilage defect | Bone marrow lesion | Osteophyte | |
| <40 years old | 4% (2-7%) | 11% (6-17%) | 14% (6-24%) | 8 (0-25%) |
| ≥40 years old | 19% (13-26%) | 43% (29-57%) | 21% (14-31%) | 37% (22-53%) |
* values are mean prevalence (95% confidence interval)
The prevalence is clearly higher in older knees.
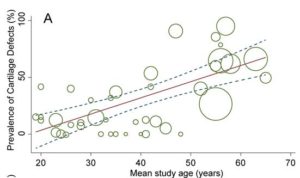
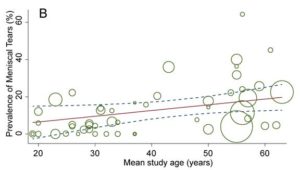
The following two figures show the prevalence of cartilage defects and meniscal tears across the lifespan. Each study is represented by a green circle (the larger the circle the more people in that study). The red line is the expected prevalence at any given age, and the dotted lines 95% confidence intervals. So, approximately 15% of all uninjured asymptomatic 30 year olds will have a cartilage defect, while this prevalence increases to approximately 60% if you are 60 years of age.
The prevalence of meniscal tears also increases as we age, but not as quickly as cartilage defects. Approximately 20% of all uninjured asymptomatic 60 year olds will have a meniscal tear.
These findings need to be considered in clinical decision making when interpreting MRI reports in patients. Just because you have cartilage damage doesn’t mean it is causing pain – many people without pain have one!